Tom's story
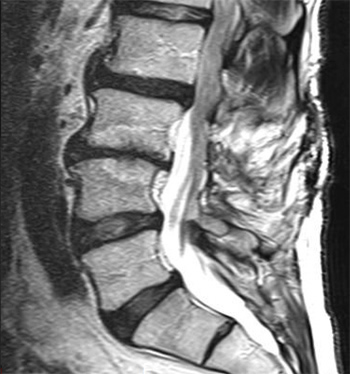
Spinal stenosis
Until he met Dr. Michael Kachmann of the Mayfield Clinic, Tom was living life in the "can't do" lane.
He couldn't lift heavy items. He couldn't sit down on the floor and get back up again. He couldn't run, and couldn't even walk more than two city blocks. "I didn't socialize," Tom says. "We never went out. Everyone knew me as the guy who was bent over and whose face showed he was in pain. I had to close my law office downtown after 41 years and move into my basement, partly because I had trouble getting in and out of my car and going back and forth to the courthouse."
Tom also knew that the "can't-do" lane was headed toward a dead end. Over the last 13 years he had been through eight spinal surgeries – six lumbar, two cervical -- in the Dayton, Ohio, area where he lived, and his options were rapidly diminishing. His Dayton surgeon had recently suggested a more radical procedure that included the insertion of rods and screws. "But I wasn't going to do that," Tom says.
It was late 2014 when, "as a last resort," Tom called the Mayfield Clinic in Cincinnati. He and his wife, Elma, drove down and discussed their options with Dr. Charles Kuntz, a specialist in complex spine. Tom was still mulling over Dr. Kuntz's plan when the neurosurgeon passed away suddenly only a few weeks later, in February 2015.
Unsure where to turn, Tom scheduled an appointment with a prominent physicians group in Columbus, Ohio. He left disappointed. "All they wanted to do was give me narcotics patches and drugs, and I'd had enough of that," Tom says.
Then, to his surprise, he received a call from Dr. Kachmann, a spine specialist who had joined Mayfield earlier that year. "He thought he could help me," Tom recalls. "It was the best thing that ever happened to me."
A long history of back pain
Tom, who was in his mid-60s, had a long history of back pain. He had played football in high school and had been an ambitious runner. "I don't think I had a specific injury," he says. "I just don't think my parts fit together. It was like having healthy teeth that don't fit in your mouth, so you need braces. I didn't have enough room in my spinal column for the nerves to pass through cleanly.
"My father took me to the Cleveland Clinic because I was having trouble getting around, and I was having a lot of pain in my legs. All they had back then were x-rays. They had no MRI's. The word stenosis never came up as a diagnosis, but in retrospect I had symptoms of stenosis. I quit athletics and wore an old corset for a year and a half – something like what women used to wear in the 19th century. It had big steel rods on the outside. Eventually, that took care of my problems."
Years later, after Tom had turned 50, his spinal problems returned with a vengeance. He underwent fusion in his cervical spine and one surgery after another in his lumbar spine. "The lumbar surgeries worked only temporarily, and the symptoms always returned in weeks or months," Tom says. "And they got worse. I found it difficult to walk two city blocks. I was stooped and contorted. There were, of course, the pain medications. I was sedentary. I watched my grandchildren play from a chair. I was just miserable."
Taking a new approach
Although Tom had multiple problems up and down his spine, Dr. Kachmann's plan was to address only the area that was causing the worst of Tom's pain and discomfort: an L3 radiculopathy, where bone and disc material were pressing on the spinal nerve. Dr. Kachmann also agreed to Tom's request that he avoid inserting metal rods and screws.
"Tom had been around to many different physicians, getting multiple opinions, and he really wanted to avoid the large multilevel fusion operation," Dr. Kachmann recalls. "I saw him and examined him and thought he had an L3 radiculopathy as his main pain complaint. My father taught me to treat people, not films. So I examined him prior to looking at the films, as I do with all of my patients. I knew after examining him that I was looking to fix an L3 radiculopathy.
"This allowed me to home in on the problem that I felt could be fixed with a one-level surgery versus a larger, more complex surgery. If I had just looked at his films, it would have been easy to recommend a much larger surgery. Tom does have other areas of stenosis and degenerative changes that may be a problem in the future. However, he was symptomatic from one level.
"I offered him a minimally invasive lateral approach for an L3-4 stand-alone cage without posterior instrumentation. There is some risk with this, but the biomechanical stability of the cage alone is good. It is much better with the screws, but good without them. I felt leaving them out is a plus because it then leaves open other minimally invasive options to treating any other spinal issues that may arise in the future from his other areas of spinal pathology."
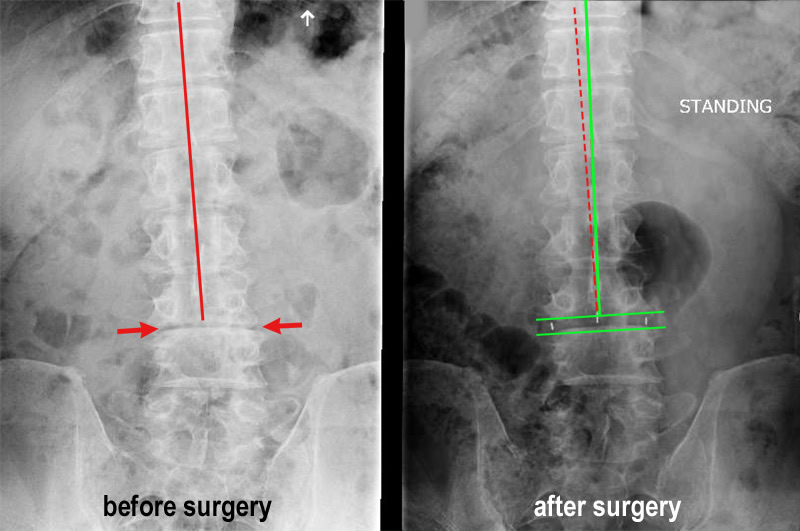
After several consultations, Tom underwent surgery in May 2015 at Bethesda North Hospital.
During the procedure, Dr. Kachmann approached the disc space in Tom's lower back from the side. He made a two-inch incision, removed the degenerated disc, and inserted a cage packed with porous bone into the empty disc space. Over time, new bone would grow through the holes in the cage, fusing the vertebrae together.
Tom, who had arrived for his surgery at 6:30 a.m., was home in Dayton for dinner.
Tom and Dr. Kachmann agree that Tom had "a few hiccups in the road after surgery," mainly because he felt so good that he overdid it. "But he has recovered very well," Dr. Kachmann says.
Today, Tom's back occasionally reminds him – with a twinge -- that his 13 years of suffering caused some permanent nerve damage. But overall, he can do almost everything he wants. He rides a stationary bike 45 minutes every day, takes three-mile walks without discomfort, and plays with his grandchildren on the floor. "I never thought I'd have my life back," Tom says. "People who see me for the first since time since my surgery say, ‘What happened to you?' Nobody can believe how quickly I turned around."
His wife, Elma, echoes his sentiments. "His back is really different; he looks different," she says. "His face is different. He has that twinkle back in his eye."
Since his surgery, Tom has referred a dozen people to Dr. Kachmann.
"We felt so simpatico with him," Tom says. "He's so easy-going, so friendly. He's professional and personable, and he talks your language.
"What is also so remarkable is that he did what I asked him to do -- as little as possible -- and it's holding up fine. I don't think anyone could have fixed it any better. People generally think that all medical care can be applied to algorithms. I have concluded that the practice of medicine, like the practice of law, is as much a work of art as it is anything else."
And when the artist is working on a patient's spine, that can make all the difference.
"When you don't have your lower back," Tom reflects, "it can seem as if you don't have much of anything."

"The result of the surgery is best displayed in this picture," Tom says. "I am an amateur American historian, and I always wanted to travel to Fort Ticonderoga in upper New York State. In September, four months out of surgery, my wife, Elma, and I decided to go. Instead of going directly to the Fort, we decided to go to the top of Mt. Defiance, which overlooks it. It was from this point in 1777 that British guns pounded the Fort below, driving the Continentals south to Saratoga and marking the great turning point of the American Revolution. We were unaware that the top was closed to motor vehicles. Therefore, the last mile and 900 feet of elevation was to be on foot. It was a tough climb, but it was the climb of my life. This picture, taken by my wife, is at the top of Mt. Defiance, four months after the surgery." Says Elma, "He was ecstatic. He never thought he could do that. He was like Rocky in the movie, running up the steps of the Philadelphia Museum of Art."
Hope Story Disclaimer -"Tom's Story" is about one patient's health-care experience. Please bear in mind that because every patient is unique, individual patients may respond to treatment in different ways. Results are influenced by many factors and may vary from patient to patient.