
Cassie's story
Pituitary tumor
There were symptoms, but Cassie didn't see them. She went up half a shoe size, but she figured she was just losing her arches. The tissue on her hands and fingers increased, but she figured she had just gained some weight. She seemed to be sweating easily, but she figured she just ran warm.
Says Cassie: "I had no inkling whatsoever that anything was wrong."
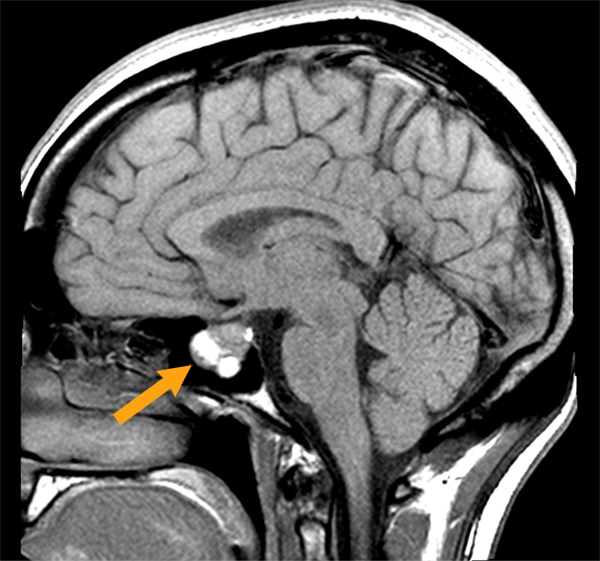
Only by accident did Cassie discover that she had a tumor on her pituitary gland that was causing excessive production of growth hormone, a rare condition known as acromegaly. An MRI scan following a concussion from a fall revealed the 2 cm tumor.
Following her diagnosis, Cassie learned that one out of every five people has a pituitary tumor, but that few of these tumors ever require treatment. Nevertheless, she was advised to see a surgeon to determine her best path forward.
A native of northeast Ohio now living in the Cincinnati area, Cassie wasn't sure where to turn. "But when people found out I had a brain tumor, they all said Mayfield is where you want to go," she says. "While talking to my primary doctor about possible surgery, she said her friend's husband, Dr. Yair Gozal, was a neurosurgeon at Mayfield. I'm a big believer in everything happens for a reason. As it turned out, Dr. Gozal specializes in pituitary tumors! Life works in mysterious ways. It definitely felt like the pieces were falling into place."
Cassie's first meeting with Dr. Gozal lasted an hour. They discussed various treatments, including medication, surgery, and radiation. They discussed the benefits and risks of removing the tumor surgically as well as the risks of not removing it. If the tumor were allowed to continue to grow, for example, Cassie risked developing more serious complications, including type 2 diabetes, sleep apnea, high blood pressure, strokes, severe arthritis, and increased size of internal organs, including the heart.
Dr. Gozal encouraged Cassie to discuss the situation with her endocrinologist, but by the end of their meeting she had already made up her mind. "I told him, 'I'm doing this.' So I signed the consent form for surgery before I left that first day. I did not need any more convincing."
Transsphenoidal approach to the tumor
Working together, Dr. Gozalimg-fluids, an ENT surgeon, performed an endoscopic transsphenoidal resection of Cassie's pituitary tumor at Good Samaritan Hospital. Dr. Isaacs began the procedure by inserting a long, tube-like instrument with a light and tiny camera into one of Cassie's nostrils. He then made an incision at the back of the nasal cavity and continued toward the tumor through the sphenoid sinus, an air-filled bony cavity deep in the nose to reach the pituitary gland and tumor. The tiny camera relayed video to a monitor, allowing Drs. Isaacs and Gozal to visualize every step of the procedure.
Once Dr. Isaacs had exposed the tumor, Dr. Gozal took over, removing it with other long, slender instruments that were inserted into Cassie's other nostril. The entire procedure took under 2 hours.
Dr. Gozal explains, "The surgery went very well. When performed with the expertise of a fellowship-trained skull base team utilizing leading-edge technology, these surgeries tend to be quite safe and elegant." He continues, "Cassie's tumor was a functional pituitary adenoma that released growth hormone, so I knew it was critical to remove the whole tumor to get her the best outcome. We brought in a specialized angled endoscope to make sure we could get a great view to ensure any visible tumor would be removed. We were quite pleased with the resection during surgery and the postoperative MRI showed no evidence of residual tumor."
Recovery
Patients experience surgery differently, and for Cassie, recovering was more challenging than she had anticipated.
"They wanted me to walk right after surgery," Cassie says. "I told them, 'I can't even open my eyes; how do you expect me to walk? But I think that was because of the anesthesia. By the next day my eyes were open. I was nauseated for a day or two, and I could not taste anything for a few weeks. I also had a severe headache for about a month."
"I definitely underestimated my recovery," she continues. "I'm the type of person who is used to working seven days a week and always being on the go. I felt like God's message to me this year was to pause and prioritize. I chose to take six weeks off work."
During this time of recovery, Cassie's headache subsided and she gradually regained her stamina. Within two months of her surgery, everything was back to normal.
"A blessing in disguise"
Cassie's prognosis is excellent. She will undergo annual MRIs so that any tumor regrowth is spotted early, and will have regular blood draws so that her endocrinologist can monitor her hormone levels.
For Cassie, the concussion and subsequent MRI proved to be a blessing in disguise. "Finding the pituitary tumor early, before I turned 30, was a fantastic blessing," she says. "Typically you don't see signs of acromegaly until you're in your 30s or 40s. By that time, some of the negative side effects that go undetected can be much, much worse than what I experienced. You can have damage to your internal organs; your feet and hands continue to grow; and you can die an earlier death."
Cassie encourages others who are diagnosed with acromegaly to stay strong and not put off treatment. "Stick with Dr. Gozal," she says. "He'll lead you down the right path."
Hope Story Disclaimer -"Cassie's story" is about one patient's health-care experience. Please bear in mind that because every patient is unique, individual patients may respond to treatment in different ways. Results are influenced by many factors and may vary from patient to patient.

