Brooke's story
Skull base meningioma
Skull base surgery restores sight – and hope
For the first time in months, standing in front of her bathroom mirror in the fall of 2021, Brooke saw her own face.
“I just remember I looked up and the mirror was in front of me, and I’m not used to seeing anything,” she said. “All of a sudden, I could see the whole outline of my face.”
Brooke has lived through a seemingly endless cycle of surgeries to deal with brain tumors – 23 surgeries in all, starting when she was a teenager. That doesn’t count plenty of targeted radiation treatments, called radiosurgery. By 2021, a brain tumor the size of a man’s fist had encamped at the base of her skull and encircled her optic nerve, cutting off her vision and forcing her left eye to protrude. There was literally nowhere for the tumor to go. Brooke noticed that her vision was getting worse, “down to just shadows.” Within weeks, she had to temporarily step away from her job as a pediatric nurse.
Enter Mayfield Brain & Spine neurosurgeon Dr. Vincent DiNapoli, a brain tumor specialist, and Dr. Jeff Nerad, an ophthalmic surgeon at Cincinnati Eye Institute.
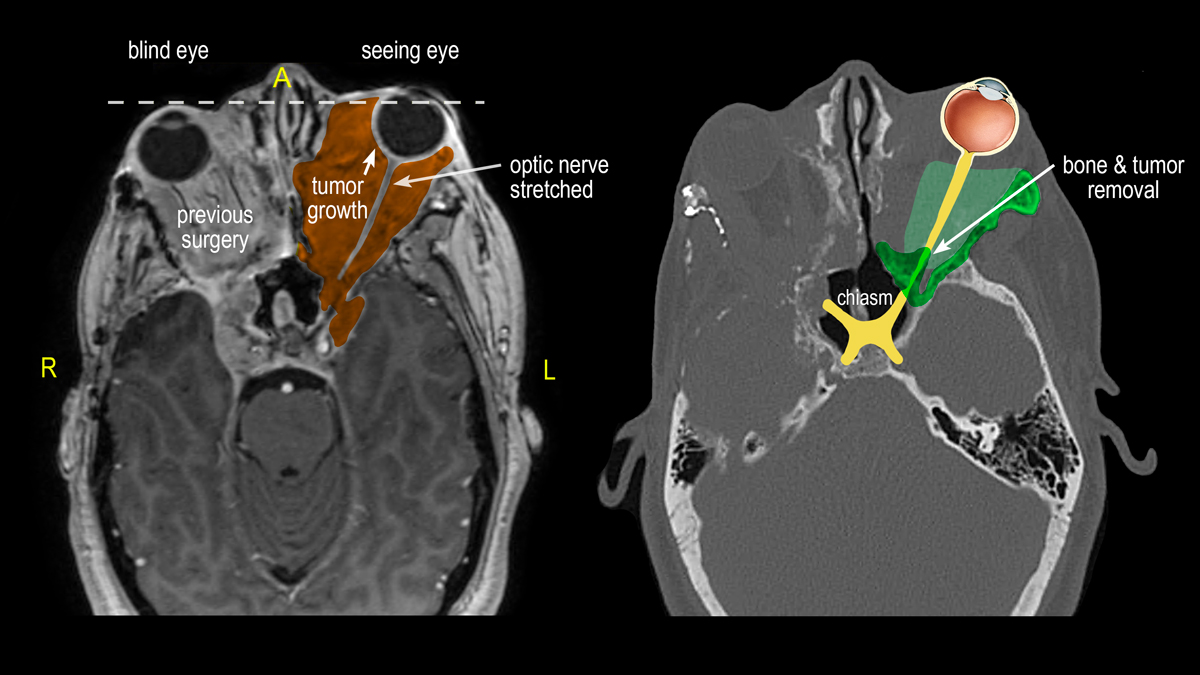
In June 2021, the two surgeons removed some of the bone off of Brooke’s orbital socket, called “decompression,” creating space for the tumor so it would put less pressure on the optic nerve.
"The entire base of her skull is tumor," Dr. DiNapoli said.
“Not too many people have such an extensive, complicated tumor,” he said. “In those situations, you have to think on your feet a little bit and say, how can we help this patient?”
That night, after the surgery, Brooke started to see flashes of light. Then on Labor Day weekend, she stood before her bathroom mirror that one morning, and she could see her face.
Brooke’s latest surgery, performed at Good Samaritan Hospital, was only the latest development in her 30-year battle against brain tumors.
She suffers from a complex meningioma, or a tumor that grows from the lining of the brain. While they are benign, meningiomas can grow through bone in the skull, making them practically impossible to remove, Dr. DiNapoli said.
Today, Brooke is back working as a nurse at Cincinnati Children’s Hospital. In October 2022, she underwent another radiosurgery procedure with Mayfield to control tumor growth. But her vision remains stable.
“My outlook is, as far as my tumors, there’s a lot of them in there, but I have this awesome medical team that’s been following me, and I have a God that has a plan, a plan bigger than mine,” she said. “I’m going to just go on with being thankful for each and every day that I have.”

Headaches started when she was 10 years old
Brooke was only 10 years old when she first started experiencing headaches. During her teenage years, she gained weight and her right eye started to protrude. It made for a difficult transition to adulthood. It also taught her that she could overcome even the most stressful challenges.
“It was hard, because physically I looked different than other kids my age,” she said. “You just kind of learn how to cope with that.”
When she was a teenager, Brooke had lost vision in her right eye. One of the tumors had encased the optic nerve leading to that eye, costing all vision on that side and leaving her with one functional eye.
Brooke’s first orbital decompression came in 1991. Then, at age 18, Brooke had her first appointment with Mayfield neurosurgeon Dr. Ronald Warnick, who would become an important provider and presence in the life of Brooke and her family.
In more than two decades since then, Brooke has undergone several craniotomies, where a neurosurgeon removes part of the skull to perform brain surgery. She has undergone multiple Gamma Knife radiosurgeries, where nearly 200 beams of radiation target tumor cells. The most recent of those have been performed at the Gamma Knife Center at The Jewish Hospital – Mercy Health, where Dr. Warnick is co-director.
“From my first meeting with Brooke, our approach has been to treat enlarging meningiomas with the optimal procedure, either Gamma Knife or surgery, with the goals of shrinking the tumor while preserving or improving function,” Dr. Warnick said. “Traditional surgery restored Brooke’s vision, and Gamma Knife radiosurgery has been instrumental in controlling numerous other meningiomas. This proves the value of a multidisciplinary approach to patients with multiple benign brain tumors.”
During the last two decades, Dr. Warnick has performed several of Brooke’s surgeries and treated her with radiosurgery as well. More importantly, he has coordinated Brooke’s care – finding specialists around the country to provide expertise, referring her to colleagues such as Dr. DiNapoli for specific procedures and nurturing her through the difficult times.
“He is ultimately who is responsible for my care and the direction of my care,” Brooke said. “He’s not always the one to do the care, but he leads me to the right person and gets things set up … I know he considers me like a daughter, and he does everything he can to basically help me survive and live.”
One of those difficult times came about a decade ago, when Dr. Warnick told Brooke that the tumor had resumed growing.
“I remember at that point just crying,” she said. “It was like, ‘This is never ever going away.’”
Brooke said she has shed plenty of tears, but she also finds opportunities to laugh and be grateful. Dr. Warnick said Brooke has approached her treatments “with extraordinary courage and enduring optimism.”

“She is a beacon of hope for other brain tumor patients and a testament to the power of prayer,” Dr. Warnick added. “I am so proud that she became a pediatric nurse and has been able to share her experiences with children who are facing their own challenges. It has been my greatest privilege to have been on this journey with Brooke.”
Brooke’s father Dale said her long battle with brain tumors has filled him with pride for his daughter.
“What’s been such a blessing is to see how Brooke has endured the illness,” he said. “… She’s had her good days and bad days like anybody, but through it all, Brooke has been a source of hope and joy and determination.”
As for Brooke, she said the endless series of treatments, of breakthroughs and setbacks, has deepened her resolve to serve other patients as a nurse.
“I really loved the nurses, and I grew very close to the nurses,” she said. “I kind of knew from age 13 or 14 that I was going to be a nurse. When I look at the kids and I look at the families, I can see a picture of what they’re going through.
“There are so many things along the way that I’ve gained,” she added. “I can really say that I wouldn’t change it. It made me who I am.”
Hope Story Disclaimer -"Brooke's story" is about one patient's health-care experience. Please bear in mind that because every patient is unique, individual patients may respond to treatment in different ways. Results are influenced by many factors and may vary from patient to patient.